Integrative Pain Management: What It Is and How It Works
Friday, Feb 13, 2026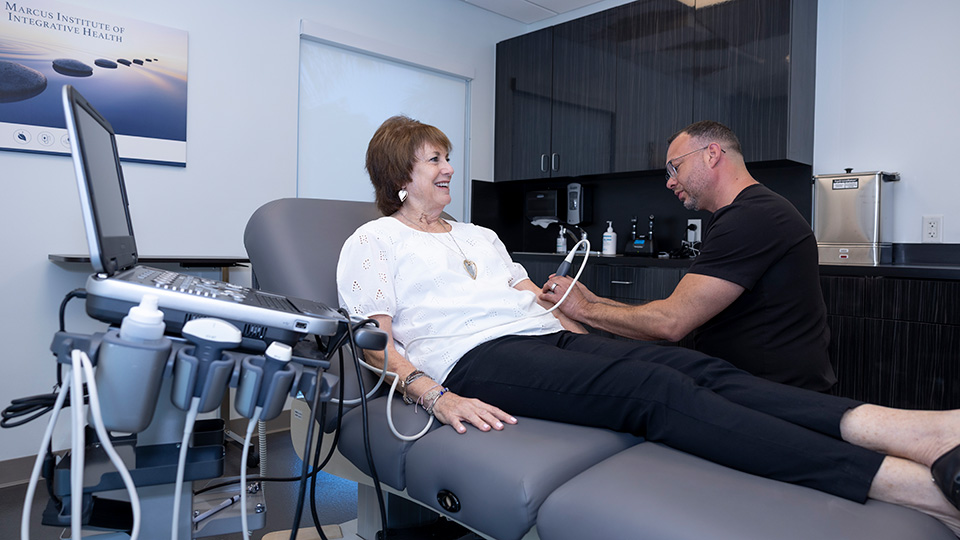
Living with chronic pain can feel like an endless cycle of frustration. Whether it’s the sharp sting of sciatica, the dull ache of lower back pain, or the burning sensation of neuropathy, pain has a way of shrinking your world.
For millions of Americans, the standard path to relief involves a revolving door of specialists and a heavy reliance on medication. This symptom-focused cycle frequently leads to an over-reliance on opioids or NSAIDs, which can carry their own risks without offering a long-term cure. But there is a different path.
Integrative pain management represents a revolutionary shift in how we understand and treat suffering. It isn't about choosing between Western medicine and alternative therapies; it's about combining the best of both worlds.
Below, we’ll talk about what integrative pain management treatment actually looks like, how it differs from traditional methods, and the specific treatment options available to help you reclaim your quality of life.
What Is Integrative Pain Management?
Integrative pain management is a coordinated, evidence-based approach to treating pain that combines conventional medical treatments with complementary therapies. While a standard pain management clinic might focus strictly on steroid injections or medication management, an integrative approach widens the lens to view the patient as a whole person.
The goal isn't to temporarily silence a symptom. It’s to achieve long-term pain relief and wellness by addressing the physical, emotional, and lifestyle factors contributing to the patient’s pain. This might mean combining advanced medical interventions—such as ultrasound-guided injections—with therapies that support the body's natural healing abilities, such as acupuncture, nutrition, and Osteopathic Manipulative Therapy (OMT) .
The Core Philosophy: Treating the Whole Person
Pain is rarely just physical. Conditions like spinal stenosis, neck pain, and joint pain don't exist in a vacuum. They’re often exacerbated by systemic inflammation, chronic stress, poor sleep, and various lifestyle factors.
If you have chronic back pain, for example, stress might cause muscle tension that worsens the pain, while inflammation from a poor diet might prevent the tissue from healing. Treating only the spine ignores the other variables that aggravate the condition.
At the Marcus Institute of Integrative Health, board-certified healthcare providers work alongside nutritionists and therapists to create personalized care plans. This model prioritizes compassionate care: providers listen closely to each individual, focusing on their experiences, health background, and unique triggers rather than rushing to a diagnosis. By treating the whole person, providers can identify root causes that traditional medicine often overlooks.
Comprehensive Treatment Options at Our Clinic
Effective treatment for chronic pain requires a diverse toolbox. Integrative pain management moves beyond the "pill for every ill" mentality, utilizing a range of modalities to restore function and well-being.
Here are some of the key tools used in a comprehensive treatment strategy.
Osteopathic Manipulative Therapy (OMT)
Movement is often the best medicine, but when you are in pain, movement can be difficult. Integrative approaches, such as OMT, use hands-on techniques to restore mobility and reduce discomfort.
OMT involves gentle pressure and movement to help doctors diagnose and treat restrictions in the musculoskeletal system. It is particularly effective for conditions like knee pain, back pain, and migraines.
Metabolic and Nutritional Support
What you eat plays a massive role in how you feel. Chronic inflammation is a common driver of pain, particularly in conditions such as arthritis and autoimmune diseases.
- Anti-Inflammatory Nutrition: Clinicians may work with you to identify food sensitivities or dietary habits that may be worsening your pain.
- Peptide Therapy: This involves using specific amino acid chains to stimulate biological processes, such as tissue repair and immune support. It’s often tailored to individual needs to enhance healing and energy.
- IM NAD (Intramuscular NAD): Delivering NAD directly into the muscle can boost energy levels and support cellular repair, which is vital for patients suffering from fatigue alongside their pain.
Mind-Body Techniques
The connection between the brain and the body is powerful. Chronic pain can rewire the brain to be more sensitive to pain signals, creating a stress-pain cycle that’s hard to break.
- Acupuncture: This evidence-based practice stimulates specific points on the body to promote natural healing and restore balance. It’s widely used for back pain, osteoarthritis, and stress reduction.
- Yoga and Meditation: These practices help calm the nervous system, reducing the "fight or flight" response that often worsens pain perception.
Advanced Medical Interventions
An integrative approach doesn’t reject modern medicine; it uses it precisely. Medical interventions are often necessary to break the pain cycle so that other therapies can take hold.
- Ultrasound-Guided Injections: Precision is key. Using diagnostic ultrasound, providers can deliver treatments exactly where they are needed—whether into joints, tendons, or around nerves.
- Regenerative Medicine: Therapies such as PRP (Platelet-Rich Plasma), A2M (Alpha-2-Macroglobulin), and Exosomes (PPX Therapy) use the body's own biological materials or signaling cells to promote tissue repair and reduce inflammation in injured joints and ligaments.
- Ultrasound-Guided SGB (Stellate Ganglion Block): This minimally invasive procedure targets a group of nerves in the neck to modulate the sympathetic nervous system. It shows promise not only for chronic pain in the upper extremities but also for alleviating symptoms of PTSD and anxiety, which often co-occur with chronic pain.
- Prolotherapy: By injecting a solution (commonly dextrose) into ligaments or tendons, this therapy stimulates the body's natural healing response to strengthen weakened tissues.
A Future Without Limitations
The journey through chronic pain can feel isolating, but integrative pain management approaches offer a bridge from suffering to a pain-free existence. By acknowledging that pain is complex and multifaceted, this approach empowers you to take an active role in your healing.
You do not have to accept pain as a permanent part of your life. Whether you’re dealing with an old sports injury, arthritis, or a complex condition like neuropathy, a comprehensive treatment strategy can help you regain your mobility and your joy.
Prioritize your well-being today. Schedule a consultation with the Marcus Institute of Integrative Health to discuss treatment plans tailored to your unique needs.
FAQs about Integrative Pain Management
- What Are the Three Types of Pain Management?
-
Generally, pain management falls into three categories:
- Acute pain (short-term, usually from injury)
- Chronic pain (lasting longer than three months)
- Cancer-related or palliative pain
Integrative care applies to all three, offering strategies to manage symptoms while promoting healing and quality of life.
- How Does Integrative Pain Management Differ from Traditional Pain Management?
-
Traditional pain management often focuses on symptom suppression, frequently utilizing medication or surgery as first-line defenses. Integrative pain management uses a holistic approach, combining conventional medical treatments with complementary therapies (such as nutrition, acupuncture, and stress management) to address the root cause of the pain and treat the whole person.
- How Effective Is Integrative Pain Management for Chronic Pain Conditions?
-
Studies suggest that combining modalities often yields higher success rates than relying on a single treatment method. By addressing the physical, emotional, and environmental factors contributing to pain, patients usually experience more sustainable relief and improved function than with medication alone.